Proton therapy decreases the chances of secondary cancers by up to 39%.
What is Proton Therapy?
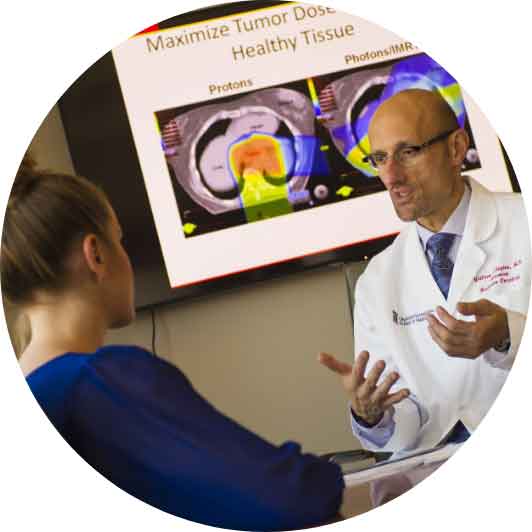
Proton therapy is an advanced form of radiation that precisely targets tumors with a maximum radiation dose that stops at the tumor site, sparing healthy tissue and organs as a result. This highly advanced technology is an effective treatment option ideal for localized, solid tumors near critical organs in the body for both adults and children with cancer. Because of the precise nature of proton therapy, it ultimately results in far fewer side effects, including secondary cancers caused by radiation. This powerful tool in the cancer fighting toolbox can help you get back to your life quicker after treatment by preserving your quality of life.
How Does it Work?
The Maryland Proton Treatment Center (MPTC) is one of only a few proton therapy facilities in the country to feature the advanced “pencil-beam scanning” technology in every treatment room. With this cutting-edge delivery technique and intensity-modulated proton therapy (IMPT), we’re able to deliver the right dose exactly where it is needed. IMPT “paints” radiation on layer by layer, hugging the tumor’s shape and minimizing the radiation dose neighboring healthy tissues receive.
Proton therapy is a painless, non-invasive, and well tolerated treatment that can be used in conjunction with other treatments, such as hyperthermia, chemotherapy, or surgery. It results in fewer side effects than traditional photon radiation and it decreases the chance of secondary cancers by 26-39%.
We are the first and most experienced proton center in the region.
Cancer Doesn’t Stand a Chance at MPTC
MPTC is the premiere proton therapy center in the Maryland, Washington DC, Northern Virginia region because of the unparalleled expertise of our world-renowned physicians and staff. As the first and only proton therapy center in Maryland, MPTC has continuously exceeded industry standards in the areas of expertise, technology, patient experience, research, and diversity.
MPTC features the most cutting-edge proton therapy technology available and is delivered by the nationally-recognized radiation oncologists from the University of Maryland.
Hear What Patients Say About MPTC
Excellence in Patient care